Improving access to women's healthcare.
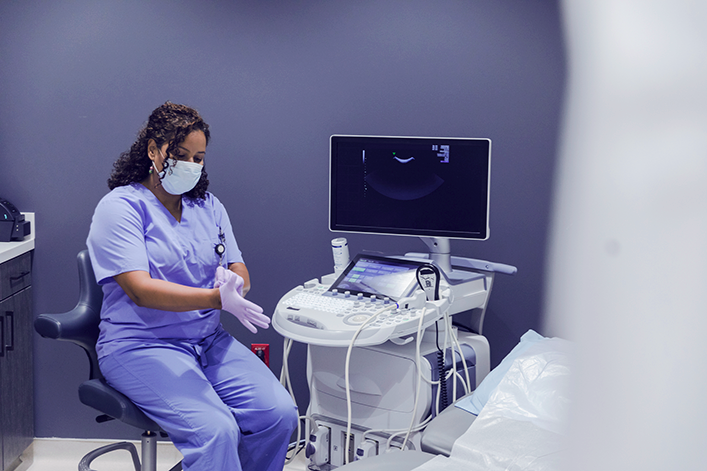
Women’s healthcare services are in demand. The average age of gynecologists is 51, and most physicians in this field retire before age 60. The potential for a shortage in the field is rising rapidly.
Thanks to innovations in health technology, women will soon have better access to healthcare and a better understanding of their health.
Protecting future mothers and current mothers-to-be.
Many women in the U.S. lack access to prenatal and postnatal care, leaving both mother and baby vulnerable to complications like:
- Preeclampsia.
- Miscarriage.
- Post-partum depression.
One of the biggest innovations in women’s healthcare is the ability to track and monitor the patient’s pregnancy from home. Technologies like ultrasounds, baby heart monitors and even app-based fertility tracking have proven to be just as accurate as instruments used in the doctor’s office.
Checkups that once were confined to the four walls of an OB’s office can now be done from the patient’s home. This move to continuous tracking and online communication lessens the risk for complications, including premature birth.
These devices even relay the information gathered back to the doctor for diagnosis and treatment. Organizations implementing these tools may see greater demand for:
- Care outside of traditional office hours.
- Remote treatment and intervention.
How will facilities manage these new demands? Cutting-edge hospitals are obtaining support from part-time or remote physicians to smooth demand and prevent burnout in their existing team.
New possibilities for parenthood.
Current advancements not only improve patient care, but also patient outcomes for both the mother and the child.
New surgical advancements mean that women who experience infertility due to cancer or other complications now have more options for IVF, including 3-D printed placenta membranes and better cryogenic egg preservation.
Women can even opt for a “womb replacement,” the total biological or lab-created reconstruction of uterine organs that allow a mother to carry a baby to term – something previously thought impossible.
Advancements like womb replacement require highly trained physicians to keep up-to-date with new technology. If a central focus of your facility is maintaining or growing market share in women’s health, consider how Baylor Scott & White Health invested in the next phase of research.
What's next for women's healthcare?
The medical advances that allow for the better care of women’s health are becoming more and more accessible to providers.
However, 49 percent of counties in the U.S. don’t have an OB/GYN – leaving almost 10 million women without the healthcare they need. Technologies like telehealth and app-based services have helped bridge the gap, but it’s only a start.
The future of women’s healthcare will depend on the adaptability of facilities and advancements within the gynecology field.
Sources: Baylor, Scott & White Health, Contemporary OBGYN, Journal of Women’s Health, MDedge, Medgadget, Science Daily


